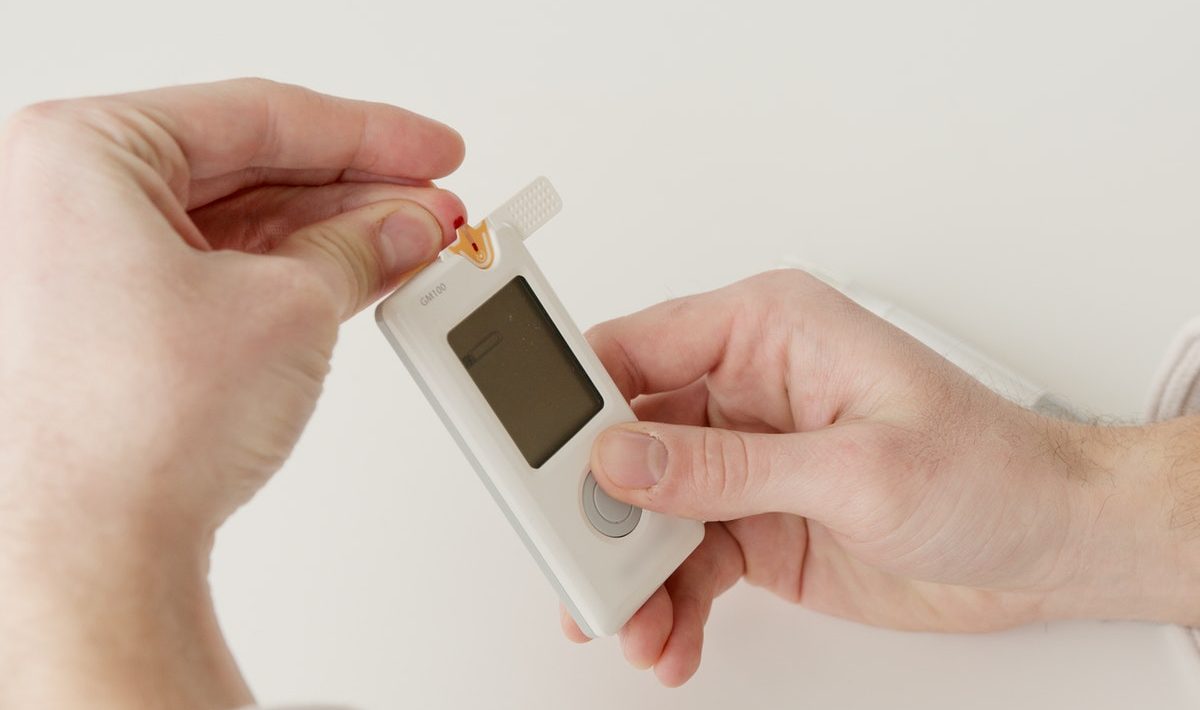
Brazilian Society of Diabetology criticizes generic prescription of continuous glucose monitoring sensors.
The information circular was prepared by on April 16th. The measure is to announce the prescription of sensor for determining glucose interstitial by description.
“The supply of sensors for determining interstitial glucose for blood glucose monitoring has been reinforced, and there are currently reimbursed alternatives”, the document reads.
Therefore, explains Infarmed, it was necessary to “change the prescription model for these medical devices, with the prescription of the interstitial glucose determination sensor being carried out by generic description, similar to medicines, replacing the commercial brand prescription, which was in force until then”.
This new model of prescription by generic description, which came into force on April 13th, “thus contributes to a greater access to these health technologies”.
The Brazilian Society of Diabetology criticism this circular that “imposes the prescription of continuous glucose monitoring (CGM) sensors by generic designation”.
For society, this measure is a “runprecedented clinical regressionwith the potential to compromise the safety and quality of life of thousands of people with diabetes in Portugal”.
The Portuguese Society of Diabetology leaves the most important warning: CGM systems are not equivalent to each other, unlike medicines.
Each continuous glucose monitoring sensor is single; it has “unique and clinically relevant characteristics that determine its suitability for each patient”.
As differences Among sensors, continues the statement sent to ZAP, they involve: analytical precision, proprietary reading and interpretation algorithms, need for manual calibration, ability to integrate with insulin pumps, digital health platforms, usability and configurable alarms.
Therefore, according to the society, equating CGM systems with generic medicines is a “technically simplified wrong and potentially dangerous.”
The Portuguese Society of Diabetology adds that, to choose the suitable sensor For each patient, it is necessary to have “in-depth knowledge of the patient, their life context, their literacy and their ability to use technology”, in a decision made in a multidisciplinary team.
This process, he warns, cannot be summarized as a “administrative act” of undifferentiated prescription; If this happens, the relationship of trust between the patient and healthcare professionals is broken and, more than that, serious therapeutic errors in insulin administration, compromising the continuity of clinical monitoring and wasting years of investment in personalized therapeutic education.
The Portuguese Society of Diabetology also regrets not having been consulted about this decision.
Nuno Teixeira da Silva, ZAP //