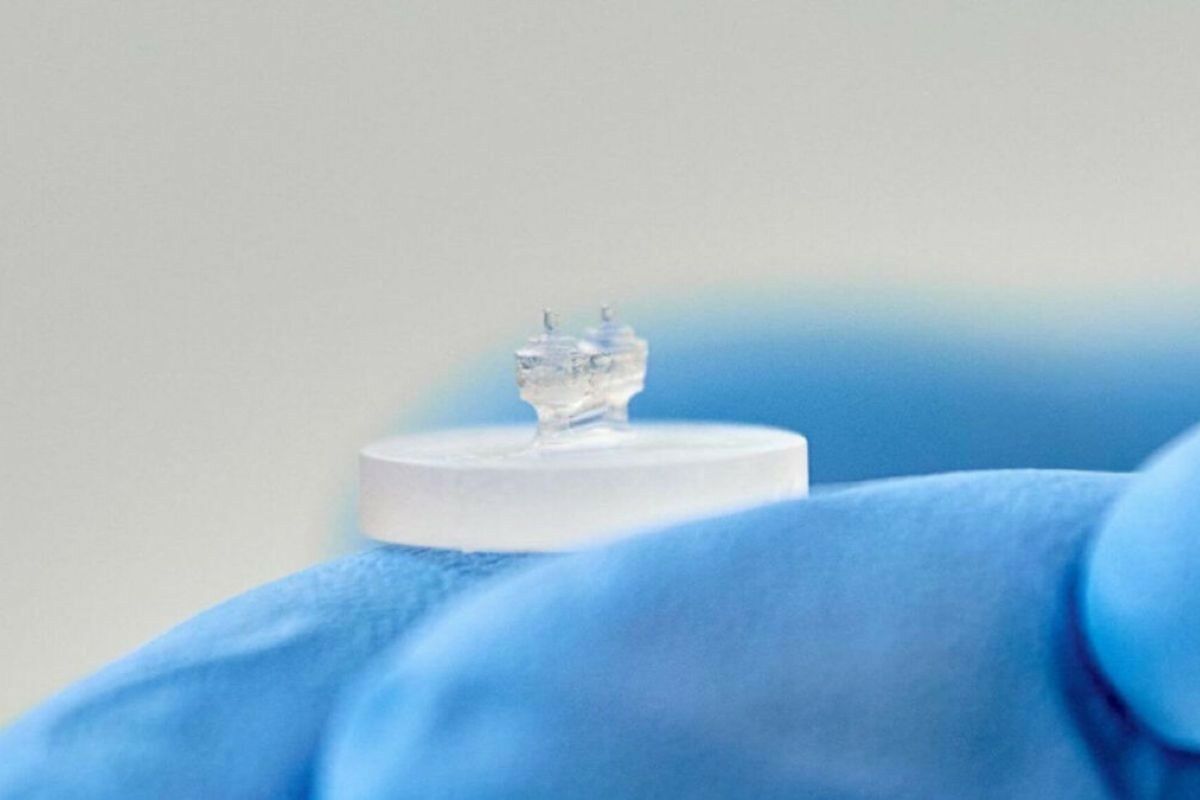
Véronique Lavoie, CHU Sainte-Justine
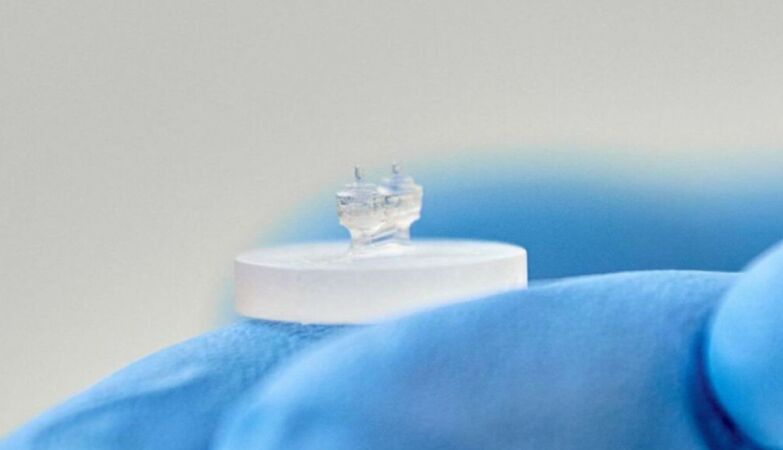
In previous research, researchers created “hearts-on-a-chip,” 3D-printed ring-shaped devices using a biological ink containing the patient’s own stem cells.
Scientists have created a three-dimensional “heart-on-a-chip” that could provide a breakthrough in the fight against cardiovascular disease.
New heart tissue just out of the lab is the first to incorporate a dual-sensing platform that allows real-time monitoring of activity throughout the heart tissue down to the cellular level.
In the article, recently in Nano Micro Smallscientists from several Canadian institutions describe how they achieved this “significant advance in cardiac tissue engineering and pharmacological testing.”
As at writes, the fundamental advance was the integration of sensors capable of detecting cardiac activity on both the macroscale and microscale.
Small-scale detection is vital because many cardiovascular diseases (CVDs) are associated with dysfunction in cardiomyocytes, the individual contractile cells that form cardiac muscle tissue, or myocardium. As a result, measuring cellular function is critical to preventing heart failure in patients with CVDs.
“Heart-on-a-chip” – what is it?
To build the three-dimensional scaffolds (HOCs), the researchers collected cardiac muscle cells and cardiac connective tissue cells from rats.
They then inserted these cells into a gel-like matrix rich in fibrous proteins and nutrients to stimulate growth, and then seeded them into small flexible silicon-based chips.
The researchers incorporated two types of sensors into their HOCs. To measure macroscale forces, they placed engineered heart tissue between two elastic pillars. These pillars deform with each heartbeat, and the amount of deformation corresponds to the contractile force throughout the tissue.
As Science Alert states, they also immersed flexible hydrogel-based microsensors inside the fabric. The deformation of these tiny droplets, averaging just 50 micrometers (0.002 inches) in size, captures local mechanical stresses at the cellular level.
Here are the two compounds
The first, the norepinephrineis also known as norepinephrine. It primes the body’s fight-or-flight response and is used in clinical settings to increase cardiac activity and maintain blood pressure, including during cardiac arrest.
To test the opposite effect and decrease contractile activity, the researchers also applied the blebbistatinaan inhibitor of muscle activity.
The drugs worked as expected, demonstrating that the HOCs can predict how cardiac force generation and heart rhythms respond to common compounds.
“The ability to observe tissue response to different compounds in real time represents a major advantage for preclinical development,” said the study leader, But Mousavibiomedical engineer at the University of Montreal, for Science Alert.
In the long term, HOCs could help doctors choose treatments based on tests performed on a patient’s own cells, before a drug is prescribed.