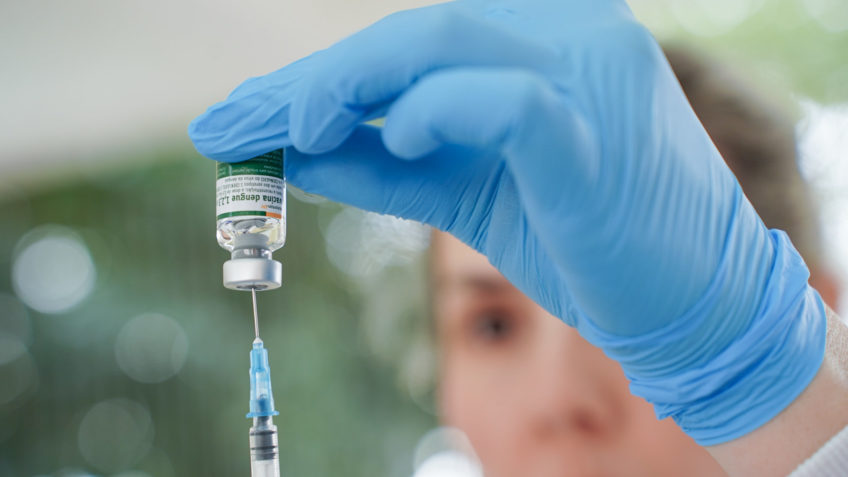
Partnership between Instituto Butantan and NIH in the USA took two decades to transform research into immunization applied in Brazil
In 2006, scientist Isaías Raw (1927-2022), former director of and , invited researchers from NIAID (National Institute of Allergy and Infectious Diseases), part of the NIH (National Institutes of Health) in the United States, to a meeting.
The reason: to understand the technology that the North American organization had been developing with a view to obtaining a vaccine candidate against dengue. That year, the disease reached historic levels in the Americas region, with 260,000 probable cases in Brazil alone, and Isaías saw the need to have a national immunizer to protect the population from dengue. 20 years and a lot of work later, Butantan-DV, developed by the Butantan Institute, reached the arms of Brazilians.
The partnership between NIH/NIAID and Butantan was made official in 2009, when the North American institute provided attenuated strains of the four serotypes of the dengue virus (DENV-1, DENV-2, DENV-3 and DENV-4) so that the vaccine could be developed in Brazil.
The licensed technology was the result of a decade of research in the USA and more than 30 phase 1 clinical trials, necessary to identify the best way to mitigate each of the 4 viruses. The objective was for all of them to provoke a satisfactory immune response, resulting in a vaccine capable of protecting against 4 types of the disease.
The senior scientist at the NIH/Niaid Viral Diseases Laboratory Stephen Whitehead, who led the development of the attenuated strains, and the scientist and director of the Johns Hopkins University Immunization Research Center, Anna Durbin, who conducted the clinical trials in partnership with the NIH/Niaid, tell the behind-the-scenes of this scientific journey and how the collaboration with the Butantan Institute over 20 years was fundamental for the vaccine to reach those who need it most.
4 vaccines in one
Developing an immunizer against dengue is an even more complex process than in the case of other viral vaccines. This is because there are 4 types of the virus and the vaccine must necessarily protect against all of them.
“If the vaccine does not induce immunity against the 4 viruses, we could end up predisposing the person to have more severe dengue fever in the future, if they become infected”said Anna.
When a person has dengue fever, they become immune to the serotype that infected them, but not to the others, and this partial immunity increases the risk of developing serious illness in a second infection.
In an attenuated vaccine, the viruses need to replicate enough to “stimulate” an infection and make the body produce antibodies, but without causing the disease. To arrive at the tetravalent formulation, it was necessary to study different ways of attenuating – or “weaken” – each virus.
The technique that worked very well for DENV-4, for example, was not effective for DENV-2. “We customized the genetic mutations for each virus in order to obtain the most satisfactory monovalent candidates. We wanted to make sure we had the most suitable strains that were safe and immunogenic.”declarou Stephen Whitehead.
Each strain was tested separately in animal models and then in humans. There were 30 clinical trials until it was possible to determine the four best candidates to compose the immunizer. For Anna Durbin, this distinguishes Butantan-DV from other dengue vaccines currently available: it went through the evaluation of multiple individual candidates and then multiple tetravalent formulations to arrive at the most promising one.
Another challenge was investigating what would be the appropriate dosage of each strain to provide protection. 4 clinical tests were carried out with just the DENV-4 component, for example, to discover the best dose. “In the case of serotype 4, we started with a quantity of 100,000 virus particles, and ended up discovering that just 1,000 particles were enough to induce a response. This was very important in terms of cost-effectiveness”explains the researcher from Johns Hopkins University.
In the final stage, North American scientists arrived at two tetravalent formulations (the so-called TV003 and TV005). To determine which would be the safest and most immunogenic to cross the finish line, a new clinical trial was conducted.
With a single dose, TV003 generated antibodies against the 4 types of dengue in 90% of volunteers and presented a better safety profile. It was based on this formulation that the Butantan Institute developed its own version of the vaccine, analogous to TV003, between 2009 and 2012, under the leadership of Neuza Frazatti Gallina, Process Development Manager at the Viral Vaccines Pilot Laboratory.
“Butantan had confidence in the product even before we had a final formulation. It is an institution that has a very consolidated history in vaccine development, and we always knew that it would be a partnership that would work”, said Stephen.
Safety differences and single dose
Concern about the safety of the vaccine, especially in people who have never had dengue, guided the researchers at NIH/Niaid and Butantan from the beginning to the end of the journey – since other vaccines available on the market began to present a risk for this population.
In the United States, Stephen and Anna’s teams developed a controlled human infection model, also called a challenge model, to confirm that the immunity conferred by the vaccine was complete and would not cause a greater risk of severe dengue fever after an eventual infection.
In Brazil, in the phase 3 clinical trial carried out with 16 thousand volunteers, half of the participants included had a history of dengue fever, and the other half had never had contact with the virus. In 5 years of follow-up, no signs of concern were observed in any of the groups, and the vaccine demonstrated high protection against severe dengue and warning signs, in the range of 90%.
Another clear advantage, according to scientist Anna Durbin, is the application of the vaccine in just one dose. “Vaccines do not protect people; what protects is vaccination. And with a single dose, the vaccine goes further – you can immunize many more people and not have to worry about them returning to the clinic to receive the 2nd dose. They will already be protected”he states.
Global impact on public health
North American scientists, who followed the study of the dengue vaccine from the embryonic stage, believe that the vaccine, combined with mosquito control strategies Aedes aegypticould significantly reduce the number of cases and hospitalizations due to dengue in Brazil in the coming years – and, in the future, in other endemic regions.
To achieve this, they point out that the vaccine must be where the disease occurs, and the collaborative agreement between NIH/NIAID and Butantan was a key part of this process. “This work went from the bench to the product and now, with the Butantan Institute, it is going further. In the last 20 years, board after board, we have been here annually and Butantan has continued to move this project forward and understand its importance, because it is an institution committed to the health of Brazilians”, highlights Stephen.
Anna reinforces that half of the world’s population lives in areas at risk for dengue fever, and that there is still a long way to go before all of these people have access to vaccination. “When we manage to immunize the entire at-risk public, I believe we will have one of the greatest impacts ever seen against a viral disease, similar to what we have seen with measles, polio and other vaccine-preventable diseases. The burden on the healthcare system will decrease dramatically.”
The researchers also highlight the importance of the volunteers in each clinical trial, who paved the way for the vaccine to leave the laboratory and reach the population with proven safety and efficacy. “These are people who donated their time, trusted investigators and believed in science. They did this for the good of public health and we owe them our thanks,” says Anna.
Butantan-DV was approved by the (National Health Surveillance Agency) in November 2025 for the public aged 12 to 59, and began to be applied in January of this year. Vaccination began in the municipalities of Nova Lima (MG), Maranguape (CE) and Botucatu (SP), in a pilot project, and was later expanded to Primary Care health professionals. Other audiences will be gradually included.
For Stephen and Anna, the expectation is that, in the future, the vaccine can also be made available to the public aged 2 to 6 years – as the age group demonstrated promising safety and efficacy results during phase 3, including in children without previous exposure to the virus.
Currently, the Butantan Institute is conducting a clinical trial to evaluate the vaccine in the population aged 60 to 79 years. Clinical tests will be carried out over the course of a year at research centers in the states of Rio Grande do Sul and Paraná.
Recognition
In the week of, Stephen Whitehead and Anna Durbin were in Brazil and were honored for their contributions to the development of Butantan-DV, alongside professionals from the Institute who also played a fundamental role in the study. The ceremony took place on Tuesday (Feb 24), at the Vital Brazil Building.
“Butantan-DV is the result of the effort not of a single person, of a single group, but of a universe of people who worked daily for two decades to make it happen. It all started with a discovery made by Stephen in his laboratory, and together we were able to take it forward and transform it into a product that will save lives”said the director of the Butantan Institute, Esper Kallás.
With information from .