Recently, in February this year, 2 simultaneous findings repositioned the debate about , an infectious viral disease caused by a virus from the same family as human smallpox. The WHO (World Health Organization) that conventional laboratory tests were unable to correctly identify. The new strain is formed by the fusion of elements from two already known genetic lineages of the virus (clades Ib and IIb), one linked to the 2022 global outbreak and the other to a more recent outbreak in African countries.
At the end of the month in which the new strain was identified, the results of a large study with the drug tecovirimat increased concern. Main antiviral used against smallpox and other similar viruses Orthopoxvirusto which the mpox virus also belongs, the medicine had been used empirically to treat the disease, especially in severe cases or in patients at greater risk of complications. Published on New England Journal of Medicinehowever, showed that tecovirimat did not reduce the time for lesions to resolve, did not relieve pain or accelerate the elimination of the virus. The result weakens one of the main therapeutic bets against the disease precisely at a time when the mpox scenario becomes more uncertain.
The study involved 344 immunocompetent adults with confirmed clade 2 mpox —mostly with mild to moderate disease— who were randomly assigned to receive oral tecovirimat or placebo for 14 days, in a randomized, double-blind study, that is, with random distribution between groups and without patients or researchers knowing who was receiving the antiviral or the placebo. The comparison showed no evidence of clinical benefit of the antiviral in relation to placebo: clinical resolution (with healing of lesions and improvement of symptoms) occurred in 83% of treated patients, a percentage practically identical to that of the placebo group, with 84%. The average difference in pain intensity was just 0.1 point on a scale of 0 to 10, and virus clearance occurred at a similar rate in both groups (Acker et al., 2026).
The finding gains even more strength when analyzed together with the , carried out in the Democratic Republic of Congo, which reached the same conclusion for clade 1. Together, the 2 trials weaken the justification for the routine use of the drug in adults. The most delicate point is that immunocompromised people, pregnant women and children – groups at highest risk – were not adequately covered in these studies. The main therapeutic gap, therefore, remains open precisely for those who may need treatment most.
Why the new strain demands attention
The WHO assesses that this strain is probably more widespread than current records suggest. This is because the 2 cases confirmed so far were detected in the United Kingdom and India, but both involve international travel history — one to an Asia-Pacific country and the other to a country on the Arabian peninsula, not publicly identified. In other words, the circulation of the recombinant already involves at least 4 countries, in 3 WHO regions, although not all of them have been named.
The new recombinant strain is worrying for a practical reason: in the 2 cases, in the United Kingdom and India, conventional PCR tests used to differentiate clades were unable to correctly characterize the new virus. Only complete genomic sequencing showed that it was not a clade (genetic lineage) already described, but a recombinant virus, .
The distinction between clades (genetic lineages) helps to determine why the new mpox strain deserves more attention. Clade IIb, associated with the 2022 global outbreak, had a lethality rate of less than 0.1% in high-income countries. Clade Ib, in turn, predominant in Central Africa, has been linked to more serious conditions, with an estimated lethality of 3% to 5% in suspected cases and rates that can reach 11% among children and immunocompromised people. This is not a marginal difference.
From January 2024 to May last year, 26 African countries reported more than 139,000 suspected cases and around 1,788 deaths.
In Brazil, there were no deaths recorded in 2024 and 2025, but the confirmation of clade Ib in São Paulo, in March 2025, changed the nature of the risk: the country stopped dealing with just the variant linked to the previous outbreak and began to live with the possibility of circulation in a form associated with more serious outcomes, .
What needs to happen now is relatively clear. Surveillance needs to incorporate genomic sequencing more systematically, because conventional PCR does not identify recombinant strains. In terms of care, measures need to be reviewed in light of the most recent evidence, as tecovirimat cannot be used routinely in immunocompetent patients, while the most vulnerable groups continue to require therapeutic alternatives and more careful monitoring. And, from a prevention point of view, vaccination of priority groups should not wait for a new outbreak to gain scale: the window to act is now.
How to protect yourself
The main form of prevention available today is vaccination. In Brazil, the immunizer offered by the SUS for priority groups is , a 3rd generation immunizer approved for mpox, which showed an estimated efficacy of 70% to 85% in preventing symptomatic cases during the 2022 outbreak, with additional benefit when applied up to 96 hours after a risk exposure. The offer has been targeted at groups with greater vulnerability or risk of exposure, such as men who have sex with men with multiple partners, sex workers, people living with HIV and health workers.
Another vaccine with cross-protection against mpox is ACAM2000, derived from immunization against smallpox. It is not part of the strategy adopted in the SUS and has more restricted use, because it is associated with more adverse effects and is contraindicated for immunocompromised people. On the horizon, developed by Moderna, it has shown promising results in animal models.
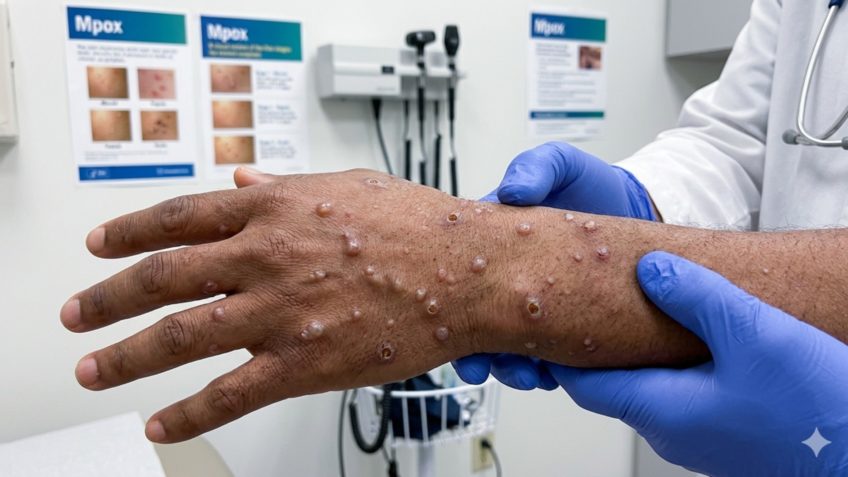
In addition to vaccination, basic prevention measures continue to apply: avoiding direct contact with skin or mucous lesions of people suspected of having mpox and seeking care if skin lesions appear, especially if they are accompanied by fever and enlarged lymph nodes after a risky exposure. In severe cases, with extensive manifestations or in patients with advanced immunosuppression, they help guide management. Studies on mpox also show why the group requires special attention.
He is a professor of Clinical Medicine and Laboratory Medicine at .
This text has been republished under a Creative Commons license. Read the original.