
Scientists developed “satellite livers” to support patients waiting for transplants: they remained viable and functional during the two months observed and produced the same types of proteins and enzymes expected from a healthy liver.
Small “satellite livers”injectable, may one day help patients with liver failure or on the transplant waiting list.
The structures developed by a team of researchers from the Massachusetts Institute of Technology (MIT) were designed to perform part of the liver’s functions without the need for invasive surgery.
Instead of replacing the diseased organ through transplantation, the team’s proposal is to inject into the body small structures made up of hepatocytes, capable of producing essential proteins and enzymes, which would function as a temporary or even lasting reinforcement of liver activity.
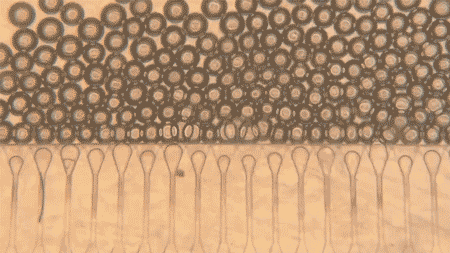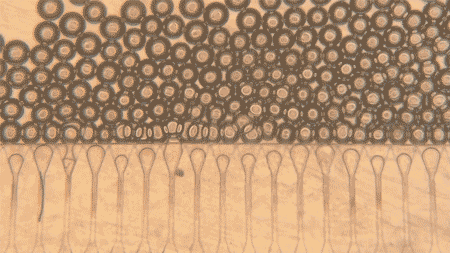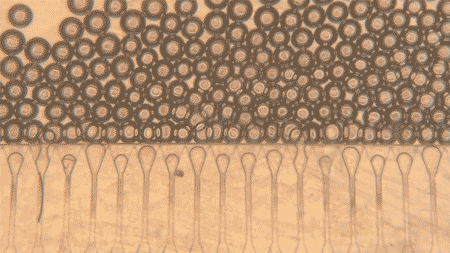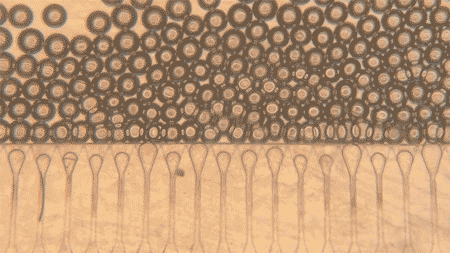
The main innovation is in the way these cells are administered. The simple injection of hepatocytes was already theoretically possible, according to the university itself, but the cells would tend to disperse and die quickly. To overcome this problem, researchers created an artificial support “niche”: hydrogel microspheres, uniform in shape and size, which function as a means of support for hepatocytes.
These microspheres can be injected into the body and, once implanted, offer enough structure to keep cells alive and functional.
In tests carried out on rats, the “mini-livers” remained viable and functional during the two months observed. Fed by the host’s blood circulation, these structures they produced the same types of proteins and enzymes expected from a healthy liver.

Scientists developed “satellite livers” to support patients waiting for transplants: they remained viable and functional during the two months observed and produced the same types of proteins and enzymes expected from a healthy liver.
Small “satellite livers”injectable, may one day help patients with liver failure or on the transplant waiting list. The structures developed by a team of researchers at the Massachusetts Institute of Technology (MIT) were designed to perform part of the liver’s functions without the need for invasive surgery. Instead of replacing the diseased organ through transplantation, the team’s proposal is to inject into the body small structures made up of hepatocytes, capable of producing essential proteins and enzymes, which would function as a temporary or even lasting reinforcement of liver activity. The main innovation is in the way these cells are administered. The simple injection of hepatocytes was already theoretically possible, according to the university itself, but the cells would tend to disperse and die quickly. To overcome this problem, researchers created an artificial support “niche”: hydrogel microspheres, uniform in shape and size, which function as a means of support for hepatocytes. These microspheres can be injected into the body and, once implanted, offer enough structure to keep cells alive and functional.
In tests carried out on rats, the “mini-livers” remained viable and functional during the two months observed. Fed by the host’s blood circulation, these structures they produced the same types of proteins and enzymes expected from a healthy liver.
According to the authors, there was also formation of new blood vessels close to the hepatocytes, which was decisive in guaranteeing the supply of nutrients and the survival of the cells, said the main author of the study on Tuesday in Cell Biomaterials, Vardham Kumar.
To researcher Sangeeta Bhatiasenior author of the study, described these structures as “satellite livers” that could provide a “reinforcement function” while the diseased organ remains in the body — “if we could insert these cells into the body, keeping the diseased organ in place.” The liver is one of the most complex and essential organs in the human body, and the shortage of organs available for transplant is increasing. The liver is involved in about 500 vital functions known, including blood clotting, blood clearance and drug metabolism. It is also distinguished by its remarkable capacity for regeneration, which is compromised in cases of liver disease, such as hepatitis or cirrhosis, when hepatocytes no longer function properly or fail to regenerate. Despite the promising results, the technology is still at a very early stage. Before any clinical application in humans, it will be necessary to evaluate the immune response, the possible need for immunosuppressive medications and the safety of the procedure in clinical trials.
[sc name=”assina” by=”ZAP” ][/sc]

The researchers used a microfluidic device to generate hydrogel microspheres with a uniform shape and size. These spheres are then mixed with hepatocytes and injected into the body, where they form stable mini-livers.
According to the authors, there was also formation of new blood vessels close to the hepatocytes, which was decisive in guaranteeing the supply of nutrients and the survival of the cells, said the main author of the study on Tuesday in Cell Biomaterials, Vardham Kumar.
To researcher Sangeeta Bhatiasenior author of the study, described these structures as “satellite livers” that could provide a “reinforcement function” while the diseased organ remains in the body — “if we could insert these cells into the body, keeping the diseased organ in place.”
The liver is one of the most complex and essential organs in the human body, and the shortage of organs available for transplant is increasing. The liver is involved in about 500 vital functions known, including blood clotting, blood clearance and drug metabolism. It is also distinguished by its remarkable capacity for regeneration, which is compromised in cases of liver disease, such as hepatitis or cirrhosis, when hepatocytes no longer function properly or fail to regenerate.
Despite the promising results, the technology is still at a very early stage. Before any clinical application in humans, it will be necessary to evaluate the immune response, the possible need for immunosuppressive medications and the safety of the procedure in clinical trials.




