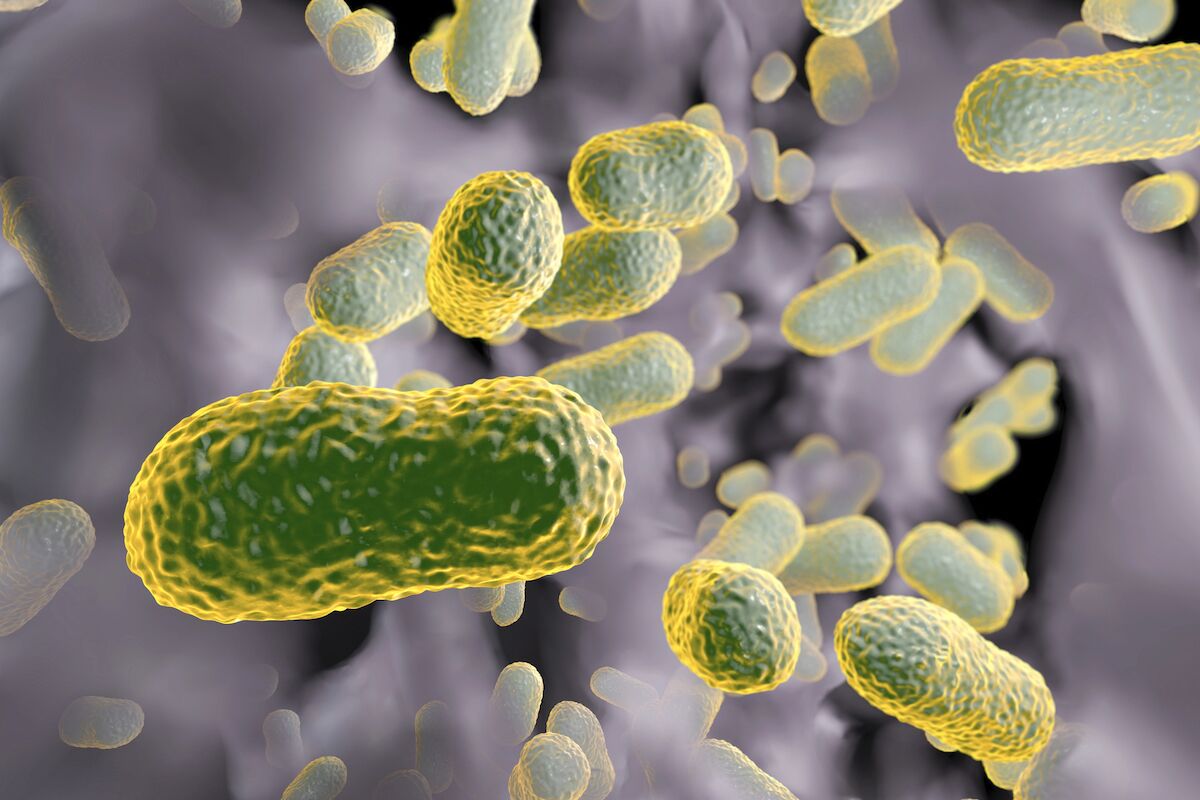
Scientists have discovered a possible vulnerability in antibiotic-resistant bacteria, including Acinetobacter baumannii (pictured), which frequently causes infections in hospital settings
In a study of mice, scientists discovered that a bacterial sugar can be exploited to deactivate antibiotic-resistant pathogens.
As resistant bacteria antibiotics can have a Achilles heel: a unique sugar molecule found only on the outer surfaces of bacterial cells. This is what a recent study in Nature Chemical Biology.
Targeting this molecule could make bacteria vulnerable to the immune system, which can then destroy germs and eliminate infections.
If the same effect can be demonstrated in humans, targeting this sugar molecule could offer a new approach to combating a wide range of superbugs — including notorious species like Acinetobacter baumannii, Helicobacter pylori e Campylobacter jejuni.
“The next phase in the development of this concept is to produce an antibody that is suitable for use in humans,” the study co-author told . Ethan Goddard-Borgerwho studies the role of sugars called glycans in disease at the Walter and Eliza Hall Institute of Medical Research in Australia.
As the same magazine writes, antibiotic-resistant bacteria represent a critical threat worldwide, and Gram-negative bacteria are a particular problem.
Bacteria within this group have tough protective layers that make them especially difficult to treat with many existing medications. Pathogens A. baumannii, H. pylori e C. jejuni belong to this group.
These bacteria often resort to a “sugar coat” to help them evade the immune system and resist the effects of antibiotics. The sugar coating essentially mimics sugars found in human cells, tricking the immune system into ignoring the bacteria.
Thank us Pse
Previous research has shown that a sugar called pseudaminic acid (Pse) It is found exclusively on the outer surfaces of bacterial cells, and it differs significantly from the sugars found in human cells.
Theoretically, this could make Pse a safe way to target infections that are resistant to antibiotics, by helping to flag bacteria as “foreign” so that the immune system can attack them.
However, previous research has been limited by the fact that scientists have had difficulty extracting enough of the sugar to study it effectively.
That’s why, in the new study, the researchers wanted to produce molecules of Pse sugar in laboratory.
The team tested these antibodies against H. pylori, C. jejuni e A. baumannii and discovered that they bound strongly to Pse in all these species bacterial. The antibodies worked even when the sugars differed in structure between bacteria.
Next, they tested sugars in mice with antibiotic-resistant A. baumannii infections. They found that tagging Pse with antibodies made infections visible to the immune system, allowing immune cells to find, engulf, and destroy bacteria.
10 mice that did not receive the antibodies died from their infections within a day. Mice treated with the antibodies had 100% survival during a full week of observation.
The study authors think that in the future, these antibodies could be given to vulnerable hospital patients to help prevent infections.
As Pse is absent in human cellshope that such a therapy would specifically target bacteria without harming healthy human cells.
In the long term, the authors propose that these antibodies could potentially be used to develop vaccines that offer broad protection against Gram-negative bacteria.