The coldest seasons of the year are traditionally marked by increase in cases of flu, infection caused by the influenza virus. Seasonality is related to the drier climate and changes in behavior typical of the cold months, such as spending more time in closed, poorly ventilated environments, which favors transmission.
Between the end of March and the beginning of April, although there is still no national consolidated number of infections in 2026. The InfoGripe bulletin, from the Oswaldo Cruz Foundation (Fiocruz), indicates an increase in cases of influenza A, with the greatest impact in the Center-South region.
According to the survey, as of April 4, more than 31,000 cases of severe acute respiratory syndrome (SARS) had already been reported this year, a clinical condition that may require hospitalization. Of these, more than 13 thousand had laboratory confirmation for , including influenza and other agents.
“The flu can progress with higher fever and complications, including bacterial infections such as sinusitis, otitis and pneumonia requiring hospitalization, exacerbation of chronic diseases, progression to severe acute respiratory syndrome and death, especially in vulnerable groups”, warns allergist and immunologist Cristina Maria Kokron, from Einstein Hospital Israelita.
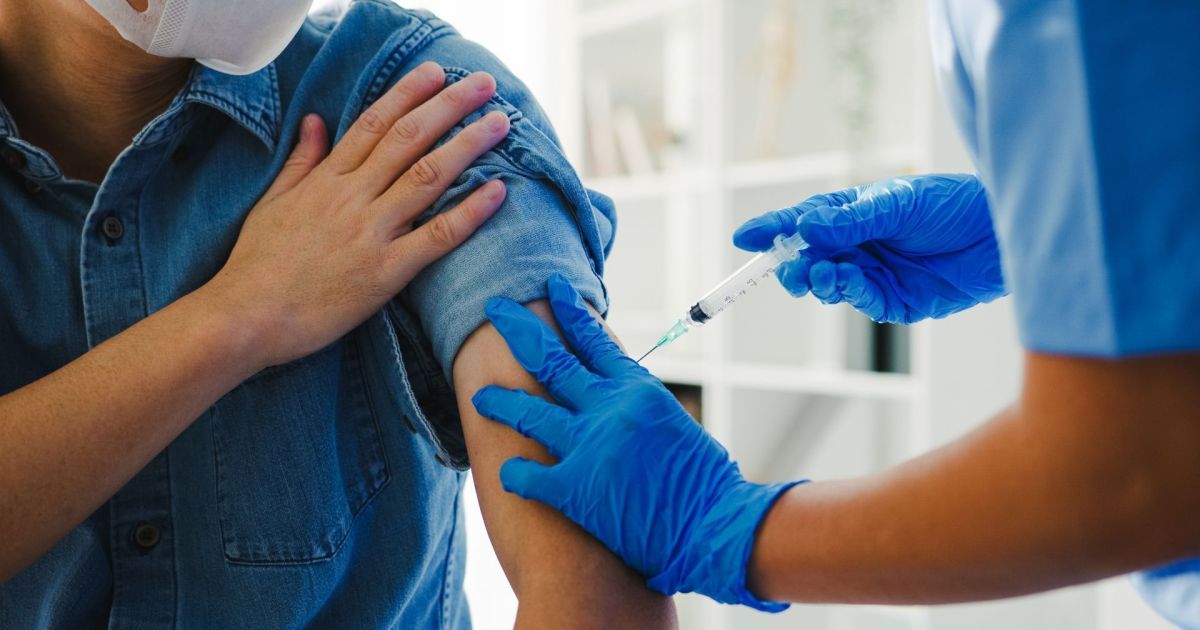
To reduce the impacts of the disease, the national vaccination campaign is carried out annually, starting in autumn, in most parts of the country. In the North region, immunization occurs in the second half of the year, before the period of greatest viral circulation, which takes place during the so-called “Amazonian winter” — characterized by a greater volume of rain and an increase in respiratory syndromes. In the case of this region, the vaccine contains the strains predominant in the Northern Hemisphere.
Old acquaintance
Despite taking place since 1999, the flu vaccination campaign is still surrounded by doubts and misinformation. One of the main concerns the need to take the vaccine every year. The influenza virus is one of the oldest infectious agents known to humanity. Widely disseminated, it has already caused major epidemics, such as the Russian Flu (1889), the Spanish Flu (1918) and, more recently, the H1N1 pandemic (2009). Today, it remains in continuous circulation and associated with mild and serious conditions.
One of the main characteristics of influenza is its high capacity for mutation. This process occurs through two mechanisms: small genetic changes during viral replication and broader rearrangements when different variants infect the same cell. These changes cause the immune system to lose, over time, the ability to recognize the virus efficiently, even in people who have had the flu or been previously vaccinated. Hence why the protection is not long-lasting.
The flu vaccine is reformulated every year, precisely to keep up with these changes. A global surveillance network monitors the circulation and evolution of strains and, based on this data, the World Health Organization (WHO) defines which variants should make up each season’s vaccines. By getting vaccinated annually, the population increases protection against the most recent viruses in circulation, reducing the risk of complications and serious forms of the disease.
In recent months, a variant known as influenza K — a subclade of (H3N2) — has caught the attention of health authorities in different countries. The increase in infections associated with this subtype sparked a global alert, and it was identified in Brazil for the first time at the end of 2025. In early April, the Ministry of Health reported having intensified epidemiological surveillance to monitor the circulation of the virus and its mutations.
Does the vaccine cause flu?
Rumors frequently circulate that the flu vaccine could cause the disease or increase the risk of infection. This is not true: the vaccine is produced with inactivated and fragmented viruses, which makes it incapable of causing flu. “The doses for influenza available in Brazil do not contain live virus, that is, they do not have the RNA, only a fraction”, explains pediatrician Alfredo Elias Gilio, coordinator of the Einstein Immunization Clinic. “I joke with my students that the virus is ‘dead and quartered,’ therefore it is impossible to cause the disease.”
Flu-like symptoms after vaccination can be caused by other infectious agents. “At this time of year, several viruses circulate with symptoms similar to the flu, which can be confused in everyday life. In general, what can happen are cases of cold caused by another group of viruses, called rhinovirus, whose symptoms are milder, such as a runny nose, cough, slight pain, low fever and malaise”, points out Gilio.
The most common adverse effects of the vaccine are mild and temporary, such as pain, redness and hardness at the application site, generally improving within 48 hours. Less frequent reactions include fever, malaise and muscle pain. Vaccination is the main way to prevent flu complications, reducing the risk of hospitalization and death.
Who can get vaccinated through SUS?
The flu vaccine offered by the Unified Health System (SUS) is produced by the Butantan Institute, in São Paulo. It is formulated in the trivalent version — that is, with three strains of the virus considered predominant in circulation around the world. Around 80 million doses are sent to the Ministry of Health, responsible for distribution to states and municipalities.
The national vaccination campaign continues until May 30 and is aimed at priority groups defined by the Ministry of Health, such as children aged 6 months to under 6 years, elderly people aged 60 or over and pregnant women. Also included are people at greater risk of exposure to the virus or worsening of the disease, such as postpartum women, indigenous peoples, quilombolas and homeless people.
Professionals considered essential, such as health workers, teachers, members of the security and rescue forces and the Armed Forces, are also part of the target audience, as well as truck drivers, public transport workers, port workers and postal workers.
The strategy also includes individuals deprived of liberty, young people undergoing socio-educational measures and people with permanent disabilities or chronic illnesses, regardless of age. “In priority populations, the vaccine is especially crucial to relieve the health system, protect the most vulnerable via collective immunity and minimize worsening of pre-existing conditions, such as heart or respiratory problems”, highlights Cristina Kokron.
In previous years, given the availability of doses, the campaign was expanded to the entire population over 6 months of age, with states and municipalities having the autonomy to include new audiences depending on stock. Therefore, after the official end of the campaign, it is common for city halls to announce the so-called “vaccine xepa”, opening up immunization to more people.
The vaccine is also available on the private network, with prices ranging between R$75 and R$230. In these cases, the most common version is the quadrivalent, which includes an additional strain of the influenza B virus. But both the vaccine offered by the SUS and the private network are effective in preventing serious cases. “The trivalent vaccine has the same range of protection as the tetravalent vaccine”, assures doctor Mônica Levi, president of the Brazilian Society of Immunizations (SBIm).