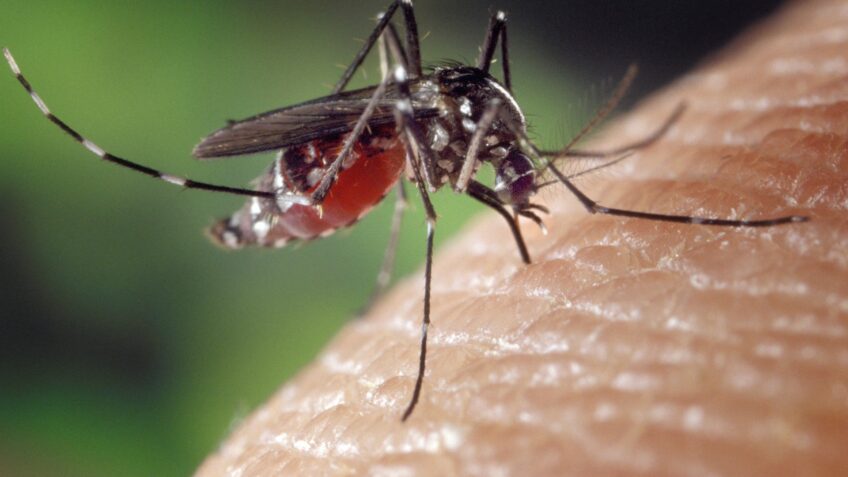
In 2024, Brazil experienced the largest dengue epidemic in its recent history, with . In 2025, there was an important reduction, with around 1.6 million probable cases by November, but the circulation of the virus remained high. For 2026, projections presented by Fiocruz indicate that dengue will still continue to affect many people in Brazil, with approximately .
The majority of infected people in the country showed the most well-known signs of dengue, such as fever, body aches, malaise and red spots. A small number of patients, however, also developed a rare neurological complication: Guillain-Barré syndrome (GBS). It was this association that we examined in a study recently published in the scientific journal .
Our study analyzed data from the SUS and showed that people with dengue have a 17 times greater risk of developing GBS in the 6 weeks following infection than in the 6 weeks after that period. To reach these results, we used 3 large SUS databases: hospitalizations, dengue notifications and death records. In total, we identified more than 5,000 GBS hospitalizations from 2023 to 2024 – 89 of which occurred shortly after a dengue infection.
Rare condition
GBS, which occurs mainly after infections, is a rare condition in which the immune system itself attacks peripheral nerves. This causes muscle weakness that starts in the legs and can move up to the arms and face. In severe cases, the person may become completely paralyzed and need help from breathing machines.
The suspicion that dengue was associated with GBS is longstanding. . However, to date, no in-depth analysis has been carried out to quantify this relationship. This is what we sought to do by gathering large national data and observing what happens in the weeks following infection.
How the study was carried out
We use an analysis strategy called “self-controlled case series,” in which each person is compared to themselves. Thus, we assessed whether the risk of developing GBS increases in the weeks after dengue by comparing the period from one to 6 weeks after the onset of symptoms with the period after 6 weeks, which served as a reference.
Our results showed that the risk of GBS increases after dengue infection, approximately 17-fold at one and 6 weeks. The risk is concentrated especially in the first two weeks after the onset of dengue symptoms, when it is approximately 30 times greater. After 6 weeks, the risk returns to the expected level.
In absolute numbers, we estimate that, for every 1 million cases of dengue, approximately 36 people develop GBS. The relationship between arboviruses and neurological complications had already emerged significantly during the Zika epidemic in 2015 and 2016. The Zika virus was associated with microcephaly in babies, but also with a significant increase in GBS cases in adults. Dengue is part of the group of arboviruses, and the virus is classified in the family Flaviviridae.
Treatment should begin as soon as possible
GBS treatment is most effective when started early.
The two main therapeutic options, both available in the SUS, are intravenous immunoglobulin and plasmapheresis. Plasmapheresis is a blood “filtering” procedure that aims to remove the antibodies responsible for attacking the nerves. These treatments are crucial to stopping the progression of the disease and speeding recovery.
The challenge is time: the sooner treatment begins, the better the results. Therefore, signs such as weakness in the legs, tingling in the feet or difficulty walking after a recent episode of dengue require medical evaluation.
Our discovery adds to a growing body of evidence about the damage caused by arboviruses, from Zika-associated microcephaly to increased . Preventing these infections means avoiding not only fever and body aches, but also these other complications.
Mosquito control Aedes aegypti and vaccination are integral parts of dengue prevention. Eliminating standing water in pots, tires and gutters continues to be an effective measure to reduce transmission. In some cities in Brazil, the release of , which interferes with the mosquito’s ability to transmit viruses and has demonstrated potential for reducing the transmission of diseases transmitted by Aedes aegypti, has also been tested.
Vaccine protection
Available in the SUS since 2024, the dengue vaccine was initially intended for . However, vaccination of adolescents has not yet reached recommended coverage. With , the Ministry of Health intends to expand the target age groups for vaccination against dengue, as a strategy to reduce cases and severe forms of the disease.
The fight against diseases transmitted by Aedes aegypti it is a global problem.
It requires the action of the government and health professionals, but also the participation of the community to improve surveillance and control of the vector and to achieve broad vaccination coverage.
Our research is part of the National Institute of Science and Technology in Digital Health (INCT DigiSaúde), supported by CNPq.
About the authors:
This text was originally published by , on April 15, 2026. The content is free for republication, citing the source, and has been adapted to the standard of Poder360.